Overview
Given the substantial burden of respiratory and critical illness worldwide and increased globalization, the Division of Pulmonary Disease and Critical Care Medicine at VCU is dedicated to research and capacity building not just in our community but globally.
The VCU - Pulmonary Critical Care Global Health Program has ongoing projects in Rwanda as well as Uganda and we have affiliations with other departments at VCU who work throughout Central and South America. Our faculty have obtained external grant funding to support research in East Africa and have published their work and presented at meetings internationally. Perhaps even more important, through support from the VCU - Department of Internal Medicine, our team has fostered bi-directional exchange with our colleagues in Rwanda, which allows our division to learn from their expertise.
While the COVID19 pandemic has created challenges within global health it has also provided opportunities, both for research, and new solutions like telemedicine to support our colleagues abroad.
Our Projects
Learn more about current projects
Our Research Publications
Project: Implementation of a Bronchoscopy Program in Kampala, Uganda
- Jackson, P., Siddharthan, T., Argento, A. C., Sachdeva, A., Yarmus, L., Gupte, A., ... & Lee, H. J. (2020). Pilot project to assess the potential cost benefit of a bronchoscopy program for the diagnosis of tuberculosis in Uganda. Chest, S0012-3692.
- Siddharthan, T., Jackson, P., Argento, A. C., Sachdeva, A., Yarmus, L., Alupo, P., ... & Lee, H. J. (2020). A Pilot Program Assessing Bronchoscopy Training and Program Initiation in a Low-income Country. Journal of Bronchology & Interventional Pulmonology.
Project: Investigating Interstitial and Restrictive Lung Disease in sub-Saharan Africa
- Jackson, P., & Siddharthan, T. (2020). The global significance of PRISm: how data from low-and middle-income countries link physiology to inflammation. European Respiratory Journal, 55(4).
- Jackson, P., Siddharthan, T., Moughames, E., Rykiel, N., Padalkar, R., Katagira, W., ... & Kirenga, B. (2020). Development and Validation of an Interstitial Lung Disease Exposure Questionnaire in sub-Saharan Africa. Chest, 158(4), A1067.
Project: Sepsis and Septic Shock in Rwanda
- Hopkinson D.A., Mvukiyehe J.P., Jayaraman S.P., Syed A.A, Dworkin, M.S., Mucyo W., Cyuzuzo T., Tuyizere A., Mukwesi C., Nyirigira G., Banguti P.R., Riviello E.D.. Sepsis in Rwanda: a retrospective cohort study on presentation, management, outcomes, and predictors of mortality. PLOS ONE. 2020, Aug; Pub Status: Under Review.
Where We Work
Learn more about our global work
Uganda
 Uganda, known as “the Pearl of Africa” is a relatively small country of approximately 43 million people in East Africa. Like many countries in sub-Saharan Africa there is an emerging convergence of communicable and non-communicable pulmonary disease challenging the health care system. Uganda is amongst the 30 countries with the highest rates of TB and HIV co-infection in the world but also has high rates of COPD, Asthma and restrictive lung disease. These challenges are being met with research from the VCU-PCCM Global Health Team and our partners at the Makerere University College of Health Sciences Lung Institute and Infectious Disease Institute.
Uganda, known as “the Pearl of Africa” is a relatively small country of approximately 43 million people in East Africa. Like many countries in sub-Saharan Africa there is an emerging convergence of communicable and non-communicable pulmonary disease challenging the health care system. Uganda is amongst the 30 countries with the highest rates of TB and HIV co-infection in the world but also has high rates of COPD, Asthma and restrictive lung disease. These challenges are being met with research from the VCU-PCCM Global Health Team and our partners at the Makerere University College of Health Sciences Lung Institute and Infectious Disease Institute.
Rwanda
 The “Land of a Thousand Hills” is the moniker given to the Republic of Rwanda, a small country in East Africa with a population of approximately twelve million. This land-locked country is known for its mountain gorillas, coffee, tea, and beautiful landscapes. Since the genocide against the Tutsi in 1994, Rwanda has seen notable economic, social, and public health gains. Critical care occurs in four tertiary referral (teaching) hospitals – three in Kigali and one in the Southern Province of Butare. ICU mortality has been shown to be high, with a recent study indicating a mortality rate of 48.7%. We are working with colleagues at the University of Rwanda College of Medicine and Health Sciences to better understand critical care in Rwanda and to improve critical care education and outcomes.
The “Land of a Thousand Hills” is the moniker given to the Republic of Rwanda, a small country in East Africa with a population of approximately twelve million. This land-locked country is known for its mountain gorillas, coffee, tea, and beautiful landscapes. Since the genocide against the Tutsi in 1994, Rwanda has seen notable economic, social, and public health gains. Critical care occurs in four tertiary referral (teaching) hospitals – three in Kigali and one in the Southern Province of Butare. ICU mortality has been shown to be high, with a recent study indicating a mortality rate of 48.7%. We are working with colleagues at the University of Rwanda College of Medicine and Health Sciences to better understand critical care in Rwanda and to improve critical care education and outcomes.
Our Team
Learn more about our Global Health Program team members

Peter Jackson, MD
Assistant Professor & Co-Director

Peter Jackson, MD
Assistant Professor & Co-Director
Internal Medicine
Division of Pulmonary Disease and Critical Care Medicine
Fax: (804) 828-9071
Email: peter.jackson@vcuhealth.org
Address/Location:
Box 980049
Richmond, VA 23298

Aamer A. Syed, MD, ME
Assistant Professor & Co-Director

Aamer A. Syed, MD, ME
Assistant Professor & Co-Director
Internal Medicine
Division of Pulmonary Disease and Critical Care Medicine
Phone: (804) 828-9071
Email: aamer.syed@vcuhealth.org
Address/Location:
Box 980050
Richmond, VA 23298
Our Collaborators:
 Stella Zawedde-Muyanja is a co-investigator on our project investigating the effect of the COVID19 pandemic on TB care in Uganda. Dr. Zawedde-Muyanja holds a Bachelor’s Degree in Medicine and Surgery (MBChB) from Mbarara University, a Master’s Degree in Public Health from Makerere University. She was awarded an Afya Bora Fellowship in Global Health Leadership in June 2016 and is currently a Fogarty Fellow undertaking her PhD studies at Makerere University. Dr. Zawedde-Muyanja has 17 years’ experience delivering public health interventions for HIV, TB and Malaria. She has spent the past eight years focused on TB, and has developed, implemented and evaluated interventions to improve TB case finding in under-served and high-risk populations and in children. Zawedde-Muyanja’s research focus is implementation and translational research in TB.
Stella Zawedde-Muyanja is a co-investigator on our project investigating the effect of the COVID19 pandemic on TB care in Uganda. Dr. Zawedde-Muyanja holds a Bachelor’s Degree in Medicine and Surgery (MBChB) from Mbarara University, a Master’s Degree in Public Health from Makerere University. She was awarded an Afya Bora Fellowship in Global Health Leadership in June 2016 and is currently a Fogarty Fellow undertaking her PhD studies at Makerere University. Dr. Zawedde-Muyanja has 17 years’ experience delivering public health interventions for HIV, TB and Malaria. She has spent the past eight years focused on TB, and has developed, implemented and evaluated interventions to improve TB case finding in under-served and high-risk populations and in children. Zawedde-Muyanja’s research focus is implementation and translational research in TB.
 Mudarshiru Bbuye received his B.S. in Medical Research and Biology at Kyambogo University and an MPH at Makerere University College of Health Sciences, he is currently a Research Fellow at the Makerere Lung Institute. He is an experienced Researcher with a demonstrated history of working in the public health and basic science research. Skilled in Good Laboratory Practice (GLP), data management, Epidemiology, Project planning, management, and implementation. Bbuye partners with the VCU-PCCM Global Health Team as the project coordinator and co-investigator on our project investigating the effect of the COVID19 pandemic on TB care in Uganda.
Mudarshiru Bbuye received his B.S. in Medical Research and Biology at Kyambogo University and an MPH at Makerere University College of Health Sciences, he is currently a Research Fellow at the Makerere Lung Institute. He is an experienced Researcher with a demonstrated history of working in the public health and basic science research. Skilled in Good Laboratory Practice (GLP), data management, Epidemiology, Project planning, management, and implementation. Bbuye partners with the VCU-PCCM Global Health Team as the project coordinator and co-investigator on our project investigating the effect of the COVID19 pandemic on TB care in Uganda.
 Dr. Trishul Siddharthan is an Assistant Professor of Medicine in the Division of Pulmonary and Critical Care Medicine at the University of Miami. He has ten years’ of experience conducting research related to risk factors, health outcomes and management of chronic disease in a range of low- and middle-income settings (LMICs). His current funded research pertains to identifying the effectiveness of treatment for chronic respiratory disease in LMICs and assessing the prognostic value of lung imaging for acute and chronic lung injury. Dr. Siddharthan has collaborated with our team on a number of projects in Uganda and continues to be a key partner to the VCU-PCCM Global Health Team.
Dr. Trishul Siddharthan is an Assistant Professor of Medicine in the Division of Pulmonary and Critical Care Medicine at the University of Miami. He has ten years’ of experience conducting research related to risk factors, health outcomes and management of chronic disease in a range of low- and middle-income settings (LMICs). His current funded research pertains to identifying the effectiveness of treatment for chronic respiratory disease in LMICs and assessing the prognostic value of lung imaging for acute and chronic lung injury. Dr. Siddharthan has collaborated with our team on a number of projects in Uganda and continues to be a key partner to the VCU-PCCM Global Health Team.
Our Rwandan Team:
- Kwame Aluamoah-Boateng, NP, PhD is Clinical Assistant Professor at University of Virginia
- Elizabeth Rivello, MD is Assistant Professor at Harvard and University of Rwanda
- Jennifer Rickard, MD is Assistant Professor at University of Minnesota and University of Rwanda
- Paulin Banguti, MD is Assistant Professor and Chief of Anesthesia at University of Rwanda
- Jean Paul Mvukiyehe, MD is an Instructor at University of Rwanda
Donations
Learn more about supporting our work
To support our work please consider donating to the VCU Global Health Fund. Donations to this fund can be made by navigating to the page and scrolling down to the VCU Global Health Fund.
Should you wish to discuss larger gifts, endowments or other ways you might support global health at VCU please contact Dr. Peter Jackson at peter.jackson@vcuhealth.org
Contacts
Pulmonary Critical Care Global Health Program
Please contact the VCU - Pulmonary Critical Care Global Health Program:
Co-Directors:
Peter Jackson, MD
Department of Internal Medicine
Division of Pulmonary Disease and Critical Care Medicine
Box 980049
Phone: (804) 828-9071
Email: peter.jackson@vcuhealth.org
Aamer Syed, MD
Department of Internal Medicine
Division of Pulmonary Disease and Critical Care Medicine
Box 980050
Phone: (804) 828-9071
Email: aamer.syed@vcuhealth.org
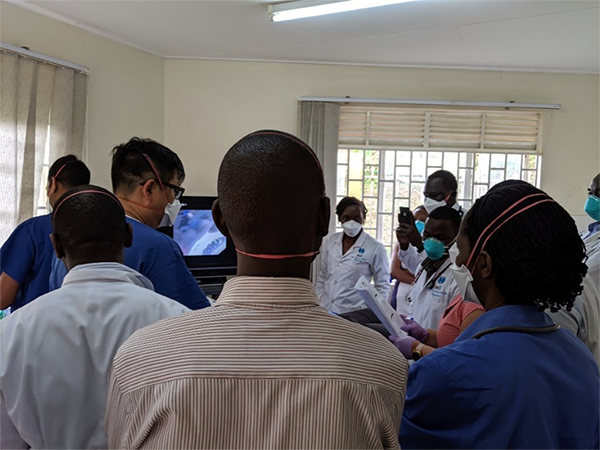 During his time at Johns Hopkins, Dr. Jackson worked alongside his colleagues Dr. Trishul Siddharthan and Dr. Hans Lee to establish the Uganda Bronchoscopy and Pleural Program (UBP) in 2019. The UBP provided equipment through donation and support from the Chest Foundation Community Service Grant and trained Ugandan clinicians to create the first public bronchoscopy program in Uganda at the
During his time at Johns Hopkins, Dr. Jackson worked alongside his colleagues Dr. Trishul Siddharthan and Dr. Hans Lee to establish the Uganda Bronchoscopy and Pleural Program (UBP) in 2019. The UBP provided equipment through donation and support from the Chest Foundation Community Service Grant and trained Ugandan clinicians to create the first public bronchoscopy program in Uganda at the  Interstitial lung disease (ILD) is a group of pulmonary disorders that are characterized by similar clinical, radiographic, and pathologic criteria. They can be caused by underlying disease or in some cases exposures that can cause inflammation and scarring in the lung. There is little data on the epidemiology of ILD in developing countries, especially in sub- Saharan Africa (sSA). Studies describing ILD in other low-middle-income countries, have shown marked differences from registries in Europe and the USA. Given that non-communicable respiratory disease is a growing global health threat and the high rates of pollution and occupational exposures in sSA it is important to characterize ILD within this region. The Global Health Team and VCU-PCCM has several projects to investigate ILD in sSA. We have developed and validated a questionnaire to assist clinicians in East Africa when they see patients with suspected ILD and two of our PCCM fellows have begun a project using telemedicine conferences to discuss cases with our international colleagues. In addition, through support from the
Interstitial lung disease (ILD) is a group of pulmonary disorders that are characterized by similar clinical, radiographic, and pathologic criteria. They can be caused by underlying disease or in some cases exposures that can cause inflammation and scarring in the lung. There is little data on the epidemiology of ILD in developing countries, especially in sub- Saharan Africa (sSA). Studies describing ILD in other low-middle-income countries, have shown marked differences from registries in Europe and the USA. Given that non-communicable respiratory disease is a growing global health threat and the high rates of pollution and occupational exposures in sSA it is important to characterize ILD within this region. The Global Health Team and VCU-PCCM has several projects to investigate ILD in sSA. We have developed and validated a questionnaire to assist clinicians in East Africa when they see patients with suspected ILD and two of our PCCM fellows have begun a project using telemedicine conferences to discuss cases with our international colleagues. In addition, through support from the  Drs. Hopkinson and Syed, Dr. Beth Riviello at Harvard Medical School, and their colleagues at
Drs. Hopkinson and Syed, Dr. Beth Riviello at Harvard Medical School, and their colleagues at  As described above in our work on sepsis in Rwanda, mortality from sepsis and septic shock is high. High-dose intravenous vitamin C when used as an adjunct has been shown to reduce mortality in sepsis; moreover, it is relatively inexpensive and may be of even greater benefit in a population with baseline nutrient deficiencies. Thus, Drs. Hopkinson, Syed, and Jackson are working with our colleagues at
As described above in our work on sepsis in Rwanda, mortality from sepsis and septic shock is high. High-dose intravenous vitamin C when used as an adjunct has been shown to reduce mortality in sepsis; moreover, it is relatively inexpensive and may be of even greater benefit in a population with baseline nutrient deficiencies. Thus, Drs. Hopkinson, Syed, and Jackson are working with our colleagues at  The FCCS course developed by the Society of Critical Care Medicine (SCCM) is widely used in the United States and provides health care professionals with an overview of various aspects of Critical Care. Internationally there is a tremendous need for such education in Low and Middle Income countries. With the support of the SCCM we have been conducting yearly courses in Rwanda with the goal of developing local instructors as well developing a course that is specifically tailored to the local environment.
The FCCS course developed by the Society of Critical Care Medicine (SCCM) is widely used in the United States and provides health care professionals with an overview of various aspects of Critical Care. Internationally there is a tremendous need for such education in Low and Middle Income countries. With the support of the SCCM we have been conducting yearly courses in Rwanda with the goal of developing local instructors as well developing a course that is specifically tailored to the local environment.